To explore more Coffee Conversations with Scientists episodes, click here.
Vasectomy surgery is an efficient and safe birth control choice for men who don't wish to father biological children. While a vasectomy is an outpatient surgery that more than 500,000 men elect to have each year in the U.S., there are still many questions and misunderstandings about what the surgery and its aftermath entail.
Jay Sandlow, MD, Chair of Urology and professor at Froedtert and the Medical College of Wisconsin discussed the science behind vasectomies–including the truth about some common vasectomy myths–in a recent episode of Coffee Conversations with Scientists.
What is Vasectomy Surgery?
A vasectomy—also referred to as male sterilization—is surgery intended to permanently prevent pregnancy. Small tubes in the scrotum, called the vasa deferentia, are cut or sealed off to prevent sperm from entering the urethra, mixing with other fluids in semen, and exiting the body through ejaculation.
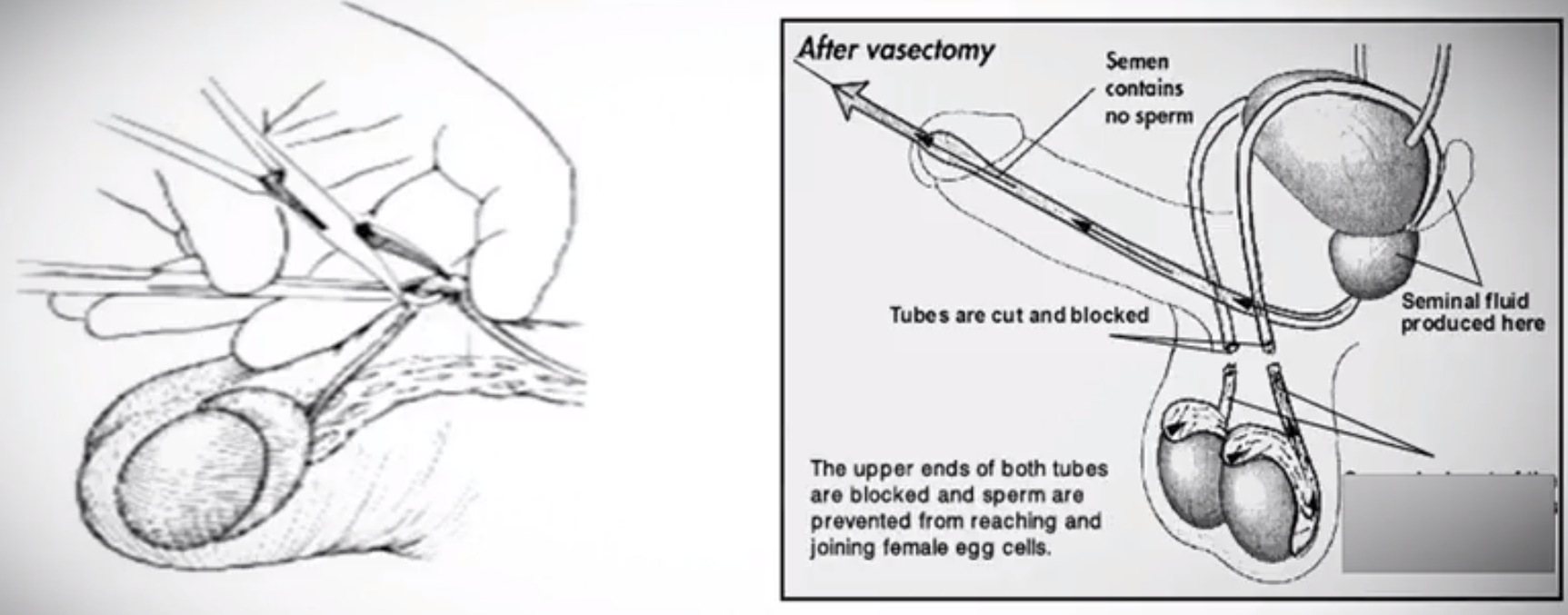
Diagram provided by Dr.Sandlow during the March 31 Coffee Conversations with Scientists Episode
According to Dr. Sandlow, "A vasectomy is the only form of male, permanent contraception. It's a blockage of the tubes carrying sperm from the testicles into the semen. It doesn't affect how the testicles work, but it prevents the delivery of sperm so that when a man ejaculates, there's no chance of pregnancy."
Vasectomy surgery, introduced in the 1800s, was used first on dogs for sterilization, and then on humans to induce prostate atrophy. It wasn't until after World War II that vasectomy surgery was recognized as a form of birth control.
Today, vasectomies are common and quick outpatient surgeries, typically taking only 10-15 minutes and requiring minimal downtime or recovery.
Who Should Have a Vasectomy?
Vasectomies are the ideal birth control option for adult men who are done having children or do not plan on fathering biological children in the future. Vasectomy surgery is considered a permanent form of contraception, though the procedure can possibly be reversed, if necessary.
Dr. Sandlow suggests that, despite the ability to reverse a vasectomy, patients should not schedule a vasectomy surgery if they think there's a chance they will eventually want to father biological children.
"I don't talk to patients about this as if it's temporary…. If patients think they want to have kids down the road, this isn't a good form of temporary form contraception because I can't guarantee they'll be able to have a successful reversal… It is not a good idea to treat it as temporary or like something they could reverse."
Why Do So Many Men Schedule Vasectomy Surgery in March?
March is a popular time of year for men to schedule their vasectomy surgery, and it has nothing to do with the season or weather.
The annual NCAA college basketball tournament, known as March Madness, is now a popular time for men to schedule their vasectomies and then rest and recover while enjoying watching the tournament games. The Oregon Urology Institute is thought to have been the first provider to promote scheduling vasectomy surgeries and suggested rest to coincide with March Madness in the late '00s.
In the years since, providers have followed suit, with some even offering pizza and other giveaways as an incentive for scheduling a vasectomy surgery during March Madness.

Addressing Vasectomy Surgery Myths
Myth: Vasectomies Impact Sexual Performance
Truth: Vasectomy surgery does not impact sexual performance or affect a man's sex drive. In fact, some studies have even shown that satisfaction increases after vasectomy surgery.
Dr. Sandlow explained, "The testosterone levels remain the same, and testosterone is the main driver for our libido, or sex drive. In terms of erections, those are controlled by nerves that are well away from where we're working (during surgery). They're more over the prostate near the bladder.
We're not doing anything in terms of a man's ability to get an erection. It’s the same thing with ejaculation: The nerves that control ejaculation are way inside our belly, nowhere near the scrotum. The only thing we're doing is putting a blockage into place. The testicles and the pituitary glands, which give the testicles signals to make sperm and testosterone, don't even know you've had a vasectomy. They're working normally."
Myth: Vasectomy Surgery is Painful
Truth: While patients might feel minor discomfort or tugging during a vasectomy, it's rare to experience severe pain during or after the procedure. Following a vasectomy, men might feel minor pain, but it can typically be aided by icing the area and taking over-the-counter pain medications such as ibuprofen or acetaminophen.
Myth: Vasectomies Are Not Effective Birth Control
Truth: Vasectomies are nearly 100% effective at preventing pregnancy, and they are the most effective method of birth control for men. After a vasectomy, it's essential to follow your doctor's instructions and return at the suggested time for semen testing. This will confirm whether there is sperm in the semen and if the vasectomy was effective.
"The failure rate for vasectomies is less than one in 2,000, and I think it's lower than that when you look at patients who follow up and get a semen analysis showing there is no sperm after a vasectomy," said Dr. Sandlow.

The Future of Vasectomy Surgery and Male Birth Control
Today, vasectomy surgery is the most effective form of male birth control available. However, the interest in exploring male contraception options is on the rise, with increasing research underway for both hormonal and non-hormonal contraceptives for men.
In the meantime, patients can be confident their vasectomy surgery will permanently stop them from fathering biological children…, and they might enjoy watching some basketball during their recovery, too.
Watch the full Coffee Conversations with Scientists episode here:




